6 Week Check – What to Expect
6 weeks is a big milestone for families and often involves a visit to the GP for baby’s immunisations and a postnatal check for both Mum and baby. We absolutely adore these visits and getting to give your baby a cuddle (pre-Covid!). This post is designed to give you an idea as to what to expect at this visit.
Logistics
Depending on your clinic, you may be encouraged to make a longer appointment as there is a lot to catch up on! Please bring your blue book. If you are planning to immunise your baby, we encourage you to give a dose of paracetamol prior to the appointment. Any documentation you receive from your birthing hospital is appreciated, as we don’t always receive this in GP land!
Mum’s Check
We will discuss your pregnancy history (if we didn’t care for you during your pregnancy), birth history and the postnatal course and your recovery. There will be questions about how feeding is going, whether it be breast or bottle feeding. If you require breastfeeding support we would encourage another hour long appointment to go over this in the detail it requires. We will discuss contraception (even though we acknowledge for some Mums that this is the last thing on your mind!) and provide information about the various options available. For some Mums their cervical screening test will be due and we will examine your perineum or abdominal wound. One of the most important parts of the consultation is mental health. Please don’t be surprised if we ask about drug and alcohol use and domestic violence, as the postpartum period is a time where Mums are particularly vulnerable and sometimes we don’t know this unless we ask. Some Mums may require follow up examinations or investigations if they had pregnancy or birth complications.
Baby’s Check
Some babies are smiling by 6 weeks and we try our best to snatch one for ourselves! We will ask about baby’s wee and poo (and we promise we won’t be grossed out if you have photos to show us!). Baby will have a full top to toe examination, including measurements of baby’s weight, length and head circumference. Common concerns that are raised at the 6 week check include:
- Rashes
- Newborn can exhibit an array of weird and wonderful rashes, most of which are completely innocent. “Neonatal toxicum” and “neonatal acne” can be seen as early as a few days old and wax and wanes over days-weeks.
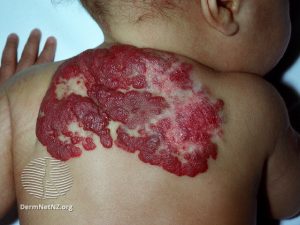 Haemangiomas or strawberry naevi occur in up to 10% of babies and involve the blood vessels under the skin. They develop shortly after birth and tend to increase in size quite quickly, most peaking at 3-5 months before slowly regressing. If the haemangioma is in a particular spot (eye, ear, lip) or very large you may be referred to a dermatologist to discuss treatment options, however most disappear on their own and can just be regarded as something that makes your baby even more special!
Haemangiomas or strawberry naevi occur in up to 10% of babies and involve the blood vessels under the skin. They develop shortly after birth and tend to increase in size quite quickly, most peaking at 3-5 months before slowly regressing. If the haemangioma is in a particular spot (eye, ear, lip) or very large you may be referred to a dermatologist to discuss treatment options, however most disappear on their own and can just be regarded as something that makes your baby even more special!- Image from Dermnet https://creativecommons.org/licenses/by-nc-nd/3.0/nz/legalcode
- “Wonky” heads
- Again, this is mostly an innocent finding. Plagiocephaly is the most common finding and presents as a flat or asymmetrical head. It occurs because baby’s skull bones are flexible and change shape easily. It can be seen from birth due to baby’s position in the uterus or events around the birth. It is useful to vary baby’s head position whilst she or he is asleep, have playtime on either sides of the baby and carry the baby on both sides to ensure that they do not spend too long in the same position. Sometimes we will refer your baby to a physiotherapist if we are concerned about the neck muscles becoming tight because baby has held their head in a particular position for too long (torticollis). Occasionally, we may feel your baby may have a different pathology to explain their misshapen head and this may require a referral to a tertiary hospital for review.
- Blocked tear ducts
- Babies have tiny tear or lacrimal ducts. Tear ducts open in the inner corner of your eye and drain to the back of the nose and throat. If they are blocked, often by a very thin membrane at the opening, tears accumulate on the surface of the eye, causing watery or discharging eyes. If the eye itself is not red, it is most likely completely benign. If the duct hasn’t unblocked itself by the time your baby is one, we would discuss referral to an ophthalmologist (eye doctor) to discuss probing the duct to open it. This rarely needs to happen. You can try cleaning the eyes with cooled, boiled water or breast milk, as well as massaging the side of the nose/inside corner of the eye with a clean finger. This is a very common problem!
- Bellybuttons
- The umbilical cord will detach by the end of the baby’s second week of life in most cases. Occasionally, it will weep/ooze afterwards and on examination we find an umbilical granuloma. It is a raw area inside the bellybutton and often looks worse than it is! It is painless, but can cause a lot of muck on baby’s clothes. We can discuss treating either with salt water or silver nitrate sticks.
- Poos
- Baby poo. We could write an (extensively illustrated) book about it! There is a huge variation in normal. Initially, we would expect babies to pass stool frequently. Stool starts as meconium (black sticky vegemite stool) before changing to dark green and then usually yellow/mustard. From day 5, you should expect about 3 stools a day at a minimum in breastfed babies. This may change quite drastically around 6 weeks in breastfed babies, as Mum’s supply adapts. Some babies go as long as 2 weeks without a poo! As a side note, our top tips for getting a breastfed baby to poo is dress in white and go out, preferably without a spare nappy!
- A lot of parents are concerned about green or mucusy stools. Sometimes there is a problem, sometimes not and your baby needs to be assessed in a holistic manner if this is a concern. Poo that is St Kilda football team colours ie red, white or black (after meconium phase passes) ALWAYS needs review.
- Foamy, frothy or explosive stools may be a sign of functional lactose overload in breastfed babies but again this needs to be assessed with a thorough history as well as observing a feed.
- Formula fed babies may exhibit a wide range of stools. Formulas that are marketed as “anti-reflux” may be thicker in consistency and slow stools down. We would generally advise picking one formula and sticking with it, rather than chopping and changing.
- Straining with poos can be common, which is known as dyschezia and an inability to coordinate the increase in intra-abdominal pressure with pelvic floor relaxation. This settles down without intervention and does not require laxatives.
- Noises
- Sometimes it is amazing how much noise such a little baby can make! Parents often report noisy or uneven breathing, particularly at night. More often than not this is normal and a product of baby’s narrow nasal passages or congestion in the nose. There are times however where a baby has “laryngomalacia” which is a “floppy airway” resulting in squeaky noise. This can worsen in the first few months of life and can generally just be monitored unless there is an issue with feeding or weight gain. If there is a pause in breathing of more than 15 seconds, with or without colour change, urgent medical review is needed.
- Vomiting
- Many parents are concerned about their baby’s vomiting. See our “gut” blog for further information about this, but essentially the valve between the stomach and oesophagus is very immature in babies and not very good at keeping milk in. Sometimes babies drink more milk than their stomach can actually hold so the excess comes up as a spill or vomit. Babies do not generally experience the discomfort that adults do when they vomit, as at less than 4 months the milk refluxed is generally pH neutral eg not acidic. If there is blood in the vomit or the baby isn’t gaining weight, this requires urgent review, as does vomiting bile. Physiological reflux settles with time as the sphincter immatures, baby is upright more often and often with the introduction of solids. We do find, however, that vomiting tends to peak at 4 months, as babies start to become more active, before improving by 6 months.
- Crying
- Crying babies are not fun. Often for the first couple of weeks, babies feed and sleep and us parents are lulled into a false sense of security. We often find at around three weeks (seemed earlier with mine!) babies “wake up” a bit more to the world and begin to cry more. We would encourage parents to draw upon the “two tools” of milk and sensory input to help settle their baby and to ensure that they can call upon support if needed. Sometimes further assessment is required to exclude a medical cause. The natural trajectory of baby crying seems to peak at 6-8 weeks before resolving around 12-16 weeks. Even if you feel like your baby just fed, try another feed as this is a huge time for growth and development and sometimes the only way to settle your baby. Of course, we would be more than happy to see families and work through their individual concerns in a Mums and Babies consultation.
Immunisations
NB This is South Australian based information and we have a different immunisation schedule to the other states
In South Australia, the routine immunisations at 6 weeks include:
- Infanrix hexa – combination vaccine – tetanus, diptheria, pertussis (whooping cough), Hepatitis B, haemophilus influenzae B, polio
- Prevenar 13 – pneumococcal
- Bexsero – Meningococcal B vaccine
- Rotarix – rotavirus vaccine
The first 3 on this list are injections, the rotarix vaccine is an oral vaccine that we squeeze into baby’s mouth.
Bexsero can cause a fever in some babies, so it is suggested that parents administer paracetamol prior to immunisations and repeat the paracetamol at 6 hours after the first dose and 6 hours after that. You do not need to wake your baby to give a dose if they are asleep, just give it when they next wake.
Any of the injections can result in a lump or redness at the injection site. Some babies have a big sleep after their immunisations, some are irritable and don’t want to feed as well. This is expected to pass in 3-5 days.
The rota virus vaccine is a live vaccine, which means it has a small amount of the virus in it. Rotavirus causes a gastro illness. We advise caregivers to ensure that they thoroughly wash their hands and dispose of nappies straight away after a nappy change to prevent them contracting the virus themselves or re-infecting their baby.
Bring along anything you need to feed your baby, as often a feed is a nice way to settle things down after immunisations.
We understand this visit can be a nerve wracking time for families and do our best to ensure it is as stress free as possible!







